Drug Pricing Transparency Trends to Watch
Written by
SmithRx
Many employers and plan sponsors today are faced with a drug pricing conundrum: they’re promised exceptional “discounts,” but their overall drug spend continues to rise. The spending trends have become untenable for employers who want to deliver sustainable value in their benefits.
In a market dominated by legacy pharmacy benefit managers (PBMs), it’s nearly impossible to parse insights into spend, as the mechanisms behind those prices remain largely obscured by complex practices, vertical integration, and opaque “handshake” deals. This puts HR and benefit teams in a tenuous position: they have to report a rise in spend that’s nearly impossible to justify to finance.
The world of healthcare and employee benefits is increasingly dynamic. New laws, new players, and new technologies are fundamentally reshaping the market. Static, year-end reports are no longer enough. Employers are no longer willing to place blind trust in their pharmacy benefit managers. Today, the conversation is shifting away from opaque reports and toward actionable, real-time insights that allow employers to take control of their pharmacy spend.
Understanding the Legacy PBM Model
To appreciate the true value of transparency, you have to first understand the fundamentally flawed mechanics of the legacy pharmacy benefits model. Most legacy PBMs operate on a system of spread pricing, where they charge an employer more for a medication than they actually pay the pharmacy to dispense it. The PBM then pockets the difference as profit.
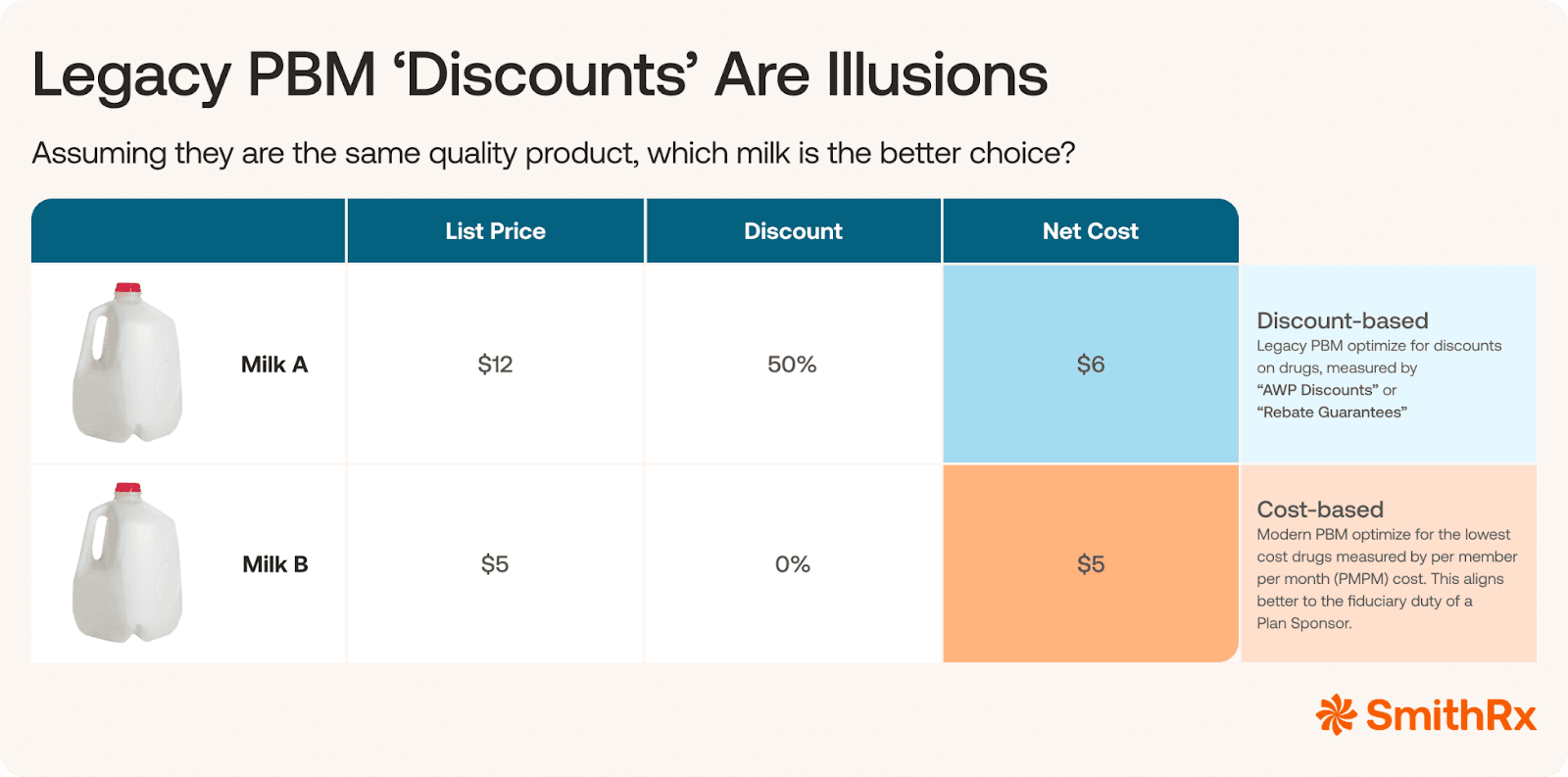
Furthermore, these models often rely on rebate-driven formularies. This model causes PBMs to prioritize a high-cost drug over a more affordable clinical alternative simply because the high-cost drug offers a larger manufacturer rebate that the PBM can then partially retain. This is also known as a “discount-based” model whereby PBMs will use higher list-price medications with steep “discounts” to make it appear as though the employer is getting a fantastic deal, but it’s still not the true benchmark cost of the medication.
This environment creates significant administrative friction for both employers and members. With legacy PBMs offering sub-par patient service, the member experience is often confusing and frustrating. For the employer, the result is a static, year-end report that shows what was spent but offers very little data on how to actually reduce costs in the future. Ultimately, these legacy models are designed to prioritize PBM revenue over employer savings, making it nearly impossible for prescribers or members to understand the true cost of care.
Defining a New Standard of Transparency
For many legacy PBMs, transparency is just a buzzword. For truly modern PBMs, transparency is part of the fundamental shift in how benefits are managed. A truly transparent pharmacy benefit manager will operate on a pass-through, cost-based model, meaning 100% of all discounts and manufacturer rebates are passed directly back to the employer.
Instead of profiting through opaque practices like drug markups or MAC list arbitrage (the practice of pocketing hidden margins by using multiple price lists for the same drug), the PBM is compensated through a simple, flat administrative fee. By utilizing a single, uniform MAC list for all clients, a modern PBM ensures cost consistency and eliminates these middleman markups. This aligns the PBM’s incentives with the employer’s goals: when the PBM doesn't profit from higher drug prices, their primary objective becomes finding the most cost-effective clinical path for the client and their members.
This model is supported by real-time cost insights and accountability across the entire supply chain. Rather than waiting a year for a retrospective analysis, employers can consistently see how their plan is performing. This allows for clinical programs to be informed by actual spend and real-world outcomes, ensuring that every dollar spent is contributing to better outcomes for their entire member population.
Head-to-Head: Modern, Transparent vs. Legacy PBMs
Legacy PBMs | vs. | Modern, Transparent PBMs |
Spread pricing and hidden fees | Pricing | Pass-through, full visibility |
Misaligned incentives and rebate volume | Decision Basis | Fiduciary alignment and cost-based pricing |
Limited insight and misaligned goals | Employer Alignment | Full insight and actionable recommendations |
Confusing and inconsistent | Member Experience | Clear and fully supported |
Unclear ROI and rising spend | Pharmacy Spend | Reduced overall spend and better member outcomes |
How Transparency Drives PBM Cost Savings
When you eliminate hidden fees and spread pricing, savings quickly follow. However, the long-term value of transparency lies in data-driven optimization. By using data, transparent, modern PBMs can optimize formularies and leverage cost-savings opportunities to steer members toward the lowest net cost medications.
This level of clarity allows employers to make smarter benefit decisions, such as identifying specialty drug trends early or adjusting plan designs to better serve their specific employee population.
Emerging Trends Supporting Transparency
We are seeing a massive surge in demand for this level of visibility. Driven by regulatory pressure, public scrutiny, and a general shift toward value-based pharmacy benefits, more employers are walking away from "black-box" contracts.
They are looking for partners who provide full visibility into drug costs and utilize advanced analytics to manage the pharmacy benefit as a strategic asset rather than an uncontrollable expense.
What Employers Should Look For in a Transparent PBM
For employers ready to make the switch, there are several key indicators of a truly transparent partner. Start by asking prospective PBMs if they allow for a full audit of 100% of claims data without restrictions. Be wary of rebate guarantees that allow the PBM to keep any excess funds, and look for a flat-fee structure that removes any incentive for the PBM to prefer higher-cost drugs.
Red flags often include vague contract language regarding "spread" or a refusal to provide analytics access. You want a PBM that is always optimizing, not one that obscures its true priorities with agreement language like “managed to contract.” In legacy PBM models, drug pricing is ‘managed to contract’ or ‘managed to guarantees’ rather than being reflective of real-time market costs.
For a deeper dive into the mechanics of ‘managed to contract’ agreements, check out this piece from the SmithRx Chief Strategy Officer, Alan Pannier.
Takeaway for Employers
The takeaway for employers is clear: the status quo is no longer sustainable. Legacy PBM models often hide costs and complicate decision-making, leaving employers to foot the bill for inefficiencies and misaligned incentives. By contrast, a transparent PBM provides the visibility and control necessary to lower costs and improve member outcomes.
At SmithRx, we have built our model on a foundation of radical transparency. By stripping away the hidden markups and providing employers with the data they need to succeed, we help organizations regain control over their pharmacy spend. Employers who adopt a transparency-first model are building a more sustainable and predictable benefit for their employees.
Learn how SmithRx helps employers reduce pharmacy spend with a transparent, data-driven PBM model.

Written by
SmithRx
SmithRx is the #1 Modern PBM, relentlessly focused on eliminating the conflicts and complexity of legacy pharmacy benefits. Built on radical transparency and fiduciary alignment, we empower employers to take control of their pharmacy spend and experience with our 100% pass-through model.



